What is PTSD?
Post-traumatic stress disorder (PTSD) is a debilitating mental condition that develops after exposure to extreme stress or a traumatic event. While the majority of people will resolve the short-term distress such an event causes, individuals with PTSD continue to be affected for much longer.
PTSD is characterized by a variety of cognitive, behavioral, and physiological symptoms related to re-experiencing the event, avoiding reminders of it, and physiological hyperarousal, such as insomnia or irritability. It is estimated that PTSD affects up to 10% of people at some stage of their lives; however, prevalence rates in people who have suffered a traumatic event may be close to 100%.

Image Credit: SpeedKingz / Shutterstock
What is cognitive-behavioral therapy?
Cognitive-behavioral therapy (CBT) has been used for the treatment of PTSD for many years. CBT aims to improve a person’s functioning by changing their patterns of behaviors, thoughts, and feelings.
CBT is based on the premise that improvements in one domain can lead to benefits in the others. For example, changing detrimental thoughts to be more helpful can help to improve a person’s mood and lead to healthier behaviors. To this end, CBT is usually administered over 12-16 sessions to an individual or a group.
CBT for PTSD
Some techniques employed by therapists when administering CBT include:
- Modifying cognitive distortions (e.g., overgeneralizing bad situations or having negative expectations) and supporting the development of more balanced and beneficial ways of thinking.
- Exposing patients to reminders of the trauma, in a controlled manner, to enable them to confront, rather than avoid, their distress.
- Educating the patient about common reactions to trauma, planning for potential crises, and teaching them to manage stress and promote relaxation
These methods are intended to help the patient with PTSD gain a more objective understanding of their traumatic experience, return their sense of control and self-confidence, and improve their ability to cope and reduce avoidance behaviors.
Cognitive Behavioral Therapy as Treatment for PTSD
Benefits of CBT
The beneficial effects of CBT are generally attributed to modifying the detrimental cognitive distortions experienced by sufferers of PTSD. The response to CBT has also been associated with physiological, functional neuroimaging, and electroencephalographic changes, including:
Related Stories
- Medical cannabis use reduces sleep disturbances caused by PTSD
- A greater decrease in heart rate reactivity and an improvement in blood pressure response on standing in PTSD patients after CBT
- Non-responders to CBT have shown significantly poorer verbal memory than responders and were also found to have impaired narrative encoding
- Motor vehicle accident survivors who received CBT had a greater reduction of right anterior activation of spontaneous electroencephalographic activity compared with controls. Across both groups, a reduction in PTSD symptoms was positively correlated with a decrease in right anterior activation to the trauma stimulus
- CBT response has been associated with functional magnetic resonance imaging (MRI) responses of the brain, with a poor response correlating with the greater bilateral amygdala and ventral anterior cingulate activation in response to masked fearful faces. This enhanced amygdala response may indicate a reduced ability to manage the anxiety reactions that CBT triggers, thus limiting response to therapy.
How does CBT Compare with other therapies?
Eye movement desensitization and reprocessing (EMDR) is another widely used therapy for PTSD with similar efficacy to CBT. This approach was originally developed by Dr. Francine Shapiro, who noticed that disturbing thoughts were alleviated by certain eye movements.
EMDR is based on the idea that negative thoughts, feelings, and behaviors are caused by inadequately processed memories. The technique requires the patient to focus on distressing images while engaging in additional bilateral sensory input, typically side-to-side eye movements.
Although generally found to be equally efficacious as CBT, controversy exists over whether the benefits of EMDR are due to voluntary eye movements that are altering the excitatory/inhibitory elements in the brain, or its similar properties to CBT, such as desensitization and exposure.
CBT has been found to be a safe and effective therapy for both acute and chronic PTSD after a variety of traumatic experiences, in adults and children, and across many cultures. CBT is associated with better remission rates as compared to other supportive therapies such as supportive psychotherapy, problem-solving therapy, present-centered therapy, psychodynamic therapy, acupuncture, hypnotherapy, and structured writing therapy.
However, studies have shown that the number of PTSD patients who do not respond to CBT can be as high as 50%. Dropouts are common, and many patients do not manage to attain remission. This may be due to a number of factors, such as other comorbid conditions like depression, and/or the nature of the study population (e.g., less education, lower level of functioning).
Over the long term, CBT improves overall symptom severity in PTSD patients as compared to non-CBT, but does not necessarily alter the overall diagnostic status of patients. Patients who receive CBT report less intense PTSD symptoms than patients who receive supportive counseling.
There is some evidence to suggest that CBT may also have preventative benefits; however, study findings are mixed, and more research is needed in this area. A review and meta-analysis recommended no use of psychological interventions following traumatic events for the prevention of PTSD. This study also indicated that interventions may have an adverse effect on some people.
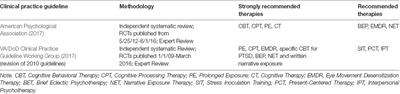
There does not appear to be a benefit in combining CBT with pharmacotherapy. The Australian Clinical Practice Guidelines for PTSD recommends that trauma-focused psychological therapy in the form of CBT or EMDR should be used over medication.
Conclusion
CBT is an effective therapy for acute and chronic PTSD, in children and adults, across many cultures, following a variety of traumatic events, with both short- and long-term benefits attributed to both psychological and neurophysiological changes.
Reference
- http://www.apa.org/ptsd-guideline/treatments/cognitive-behavioral-therapy.aspx
- http://www.ptsduk.org/what-is-ptsd/
- Shapiro F. Eye Movement Desensitization and Reprocessing, Basic Principles, Protocols and Procedures. Second edition 2001. The Guildford Press, NY, USA.
- Kar N. Cognitive behavioral therapy for the treatment of post-traumatic stress disorder: a review. Neuropsychiatr Dis Treat 2011;7:167–181.
- Syros I. Cognitive behavioral therapy for the treatment of PTSD. Eur J Psychotraumatol 2017;(sup4):1351219.
- Yehuda R. Post-Traumatic Stress Disorder. N Engl J Med 2002; 346:108-114.
Further Reading
Is CBT Effective for PTSD?
While cognitive behavioral therapy research continues to grow, it is one of the most widely-researched psychotherapy treatments and has been found to be effective in short- and long-term approaches as well as with a variety of populations, ranging from PTSD in young children to older adults.2,4
Here are several studies highlighting the effectiveness of CBT for PTSD:
- CBT has been researched and observed to be as effective as a number of other therapy types, and research indicates that it has been culturally validated across a variety of populations.
4
- Compared to a placebo, CBT was reported to be moderately helpful in treating anxiety-related disorders. The researchers did note that drop out rates were higher in PTSD samples, especially in the exposure therapy group, which infers a need for more specialized types of CBT for PTSD.
11
- A research review notes that CBT can be an appropriate, safe, and helpful intervention in the presentation of acute and chronic PTSD for people of any age.
4
- Research noted a significant improvement and significant reduction in symptoms of PTSD, in addition to feelings of depression and anxiety.
12
- After reviewing clinical trials ranging from 1980 to 2005, researchers noted that CBT had significantly maintained healthy behaviors after treatment in comparison to EMDR and therapies that are more supportive. CBT was equal to exposure therapy and cognitive therapy in reducing PTSD symptoms and the maintenance of healthy behaviors.
13
Examples of CBT for PTSD
There are a variety of CBT treatments that exist to help someone dealing with PTSD. Everyone experiences mental health differently and PTSD is not an exception to this.
Here are a few examples regarding specific treatment options as well as how they apply to each example’s experience of PTSD:
CBT for PTSD in a Veteran
Jamie, a 36-year-old Iraq war veteran, reports having had symptoms of PTSD for the past six and a half years. He continuously avoids thoughts, memories, or images (even in media) that could be connected with the experience of his fellow unit members and himself driving over an explosive device while traveling to another base.
Jamie reports a history of difficulties attending work for a number of days out of the week, repeated nightmares of the event, higher levels of depressive moods along with some irritability, and difficulty feeling connected with his spouse and other family members.
Jamie goes to 12 to 16 sessions of cognitive behavioral therapy with a focus on prolonged exposure to process these emotions and thoughts to reduce avoidance. During these sessions, the therapist assigns Jamie weekly homework assignments to regularly practice coping skills. The therapist encourages Jamie to journal his anxiety levels each day to increase awareness of stress, anxiety, and his other symptoms. In doing so, Jamie’s therapist hopes that he will increase self-expression about how he is feeling to be able to rely both on himself and a support system. This helps Jamie to monitor and reduce the impact of his symptoms by becoming aware of his warning signs and the need to initiate his coping skills.
CBT for PTSD From Witnessing Violence
Sarah, a 22-year-old who witnessed her younger brother’s murder by gunshot, has been experiencing symptoms of PTSD for 3 years. She has recurrent nightmares of the murder, and she avoids the place where her brother died and thoughts about her brother’s death. She reports continuous increasing ruminative thought and guilt surrounding her lack of protection of her brother, as well as irritability and depression throughout the year.
Sarah’s PTSD symptoms have begun to seriously impact her work relationships and with her family. After being assessed for comorbid symptoms of grief and depression in addition to PTSD, Sarah would benefit from about 12 sessions of a combination of CBT and cognitive processing therapy.
Sarah begins seeing a therapist to process her symptoms and her traumatic experience. Her therapist begins challenging her in each session to use more healthy thinking patterns and to engage in coping techniques. When Sarah’s anxiety levels rise, the therapist helps her by pointing out the unhealthy thought or increased stress response and allowing her time to practice restructuring her thoughts and engaging in a breathing activity or to relax her muscles.
Sarah’s therapist also assigns her weekly homework of journaling her anxiety and symptom levels; she is encouraged to keep practicing thought restructuring and coping mechanisms outside of sessions and to log them as well. As Sarah and her therapist work on these tasks together, Sarah begins to communicate more about her emotions and become more aware of how blaming herself impacts her thoughts.
CBT for PTSD Caused by Abuse
Bill, a 40-year-old who was physically abused by his parents until he was 18, reports a history of PTSD symptoms beginning in his early 20’s. He experienced a heightened startle reflex to any sudden movement, avoidance of talking about the abuse he experienced, constant tenseness in his body, and significant anger with people in his life.
At around 17 years old, Bill began drinking alcohol to cope with the abuse he was experiencing at home. This led to alcohol charges for a minor for which he was placed in juvenile detention. He now drinks daily, generally at least twelve 16-oz cans of beer in a day, and has been arrested for disorderly conduct. He works infrequently but in the last three months has been unsuccessfully attempting to cut back on drinking and find regular work.
Bill agrees to complete an assessment with a local therapist who is trained in trauma and substance use treatment. The therapist diagnoses Bill with PTSD and an alcohol use disorder and informs Bill that they would like to try applying acceptance and commitment therapy (ACT) in their sessions. Bill’s therapist helps him by encouraging him to accept feelings or thoughts that come up during sessions; he hopes that Bill will begin to be able to do this at home, becoming accepting of himself in and out of session.
Bill and his therapist regularly practice mindful meditation and muscle relaxation in each session, especially if Bill’s therapist notices that he’s tense, talking about drinking cravings, or having difficulty calming his anger and anxiety in session. Over time, the therapist helps Bill to become more comfortable talking about the events of his past and his feelings. Bill begins to regularly engage in coping techniques independently in and out of session; he has begun to engage in more healthy self-expression instead of letting his anger explode onto others, and reducing his drinking as his avoidance symptoms have begun to reduce by using coping techniques.
4 At-Home CBT Exercises for PTSD
While it’s always best to find a licensed therapist if you’re experiencing PTSD symptoms, the therapist may recommend some at-home exercises to keep your symptoms under control.
Here are four CBT exercises you can use at home to reduce symptoms of PTSD:10
1. Try Practicing Cognitive Restructuring on Your Own
It can be helpful to challenge or reframe your thinking in the moment on a regular basis. It can be difficult, but it’s important to challenge negative thoughts as they come up. You can also start to notice when these thoughts come up to learn what may be triggering your PTSD symptoms.
2. Practice the ABC Technique
The ABC Model allows you to explore more about how or where a negative or maladaptive belief began.
Here are the first three steps:
- Identify the (A) activating event: The trigger that would lead to a significant emotional response or maladaptive thinking
- Identify the (B) belief: The negative thought that you experienced during this trigger or event
- Identify the (C) consequences: The negative emotions or actions that happened as a result of A & B
This gives you the chance to challenge your interpretation of the trigger or belief that influenced the consequences. By engaging in this practice in a journal, you can actively track the cognitive restructuring in a more structured manner, giving you the opportunity to challenge a belief or emotional response that may have started following a traumatic event.
3. Journaling
As a follow up, keeping a journal of your thoughts, feelings, and behaviors each day may be helpful. Through writing and monitoring your thoughts and beliefs, you may begin to learn more about yourself, about the ABC’s that may be a trigger for your PTSD symptoms. You may also identify ways that have helped manage your symptoms in the past.
4. Meditation & Progressive Body Relaxation
Meditation has become highly popular in the last few years in the physical and mental health fields. When dealing with PTSD symptoms, it may be common for you to struggle with constant tenseness in your body that you feel like you can’t release.
By engaging in guided meditations, guided breathing, grounding exercises, or guided progressive relaxation, you should be able to relax your body and maybe even your anxiety levels, especially if you’ve recently experienced a trigger.